Mediterranean diet could treat depression

Colourful Mediterranean roast vegetables nestled on a bed of extra-virgin olive oil and parsley-infused quinoa, chilli beans adorned with creamy guacomale, tuna patties complemented by succulent Greek salad.
These were some simple, cheap, tasty menu items for a randomised controlled trial of Mediterranean-style diet in people suffering depression.
Results of the study, implemented by my team at the University of South Australia, Adelaide, Australia, published today in Nutritional Neuroscience, showed participants randomised to the diet group—and fortnightly cooking workshops—had greater relief from their depressive symptoms than social group attendees.
More than 80% of participants reported ‘extremely severe’ depression at study entry. After 3 months, symptom severity reduced by 45% in the diet group and 26.8% in the social group—equating to 1.68 times greater recovery in the diet group, of which 60% no longer experienced extremely severe depression. Improvements continued at 6-month follow-up.
Can a simple diet really alleviate depression? HELFIMED is one of the world’s first interventions to put this question to the test, supporting prospective population studies showing healthy diet is protective and unhealthy diet confers greater risk for depression.
HELFIMED recorded study participants’ food intake at baseline, 3 and 6 months. The diet group reported higher Mediterranean diet scores and ate more vegetables, vegetable diversity, fruit, nuts, legumes and wholegrains, and less unhealthy snacks and meat than the social group at 3 months, maintained at 6 months.
Notably, improved diet correlated with reduced depression, suggesting it indeed played a role.
The primary outcome is surprisingly similar to another Australian study published this year (compare Figures 1 and 2). That’s what you call replication.
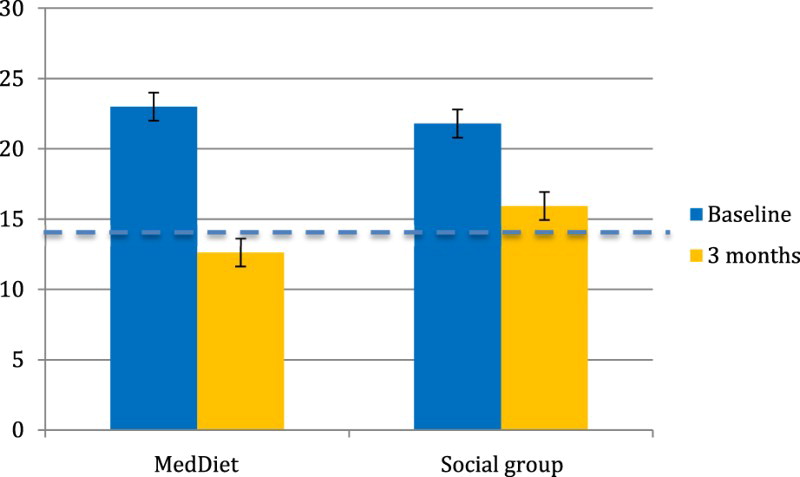
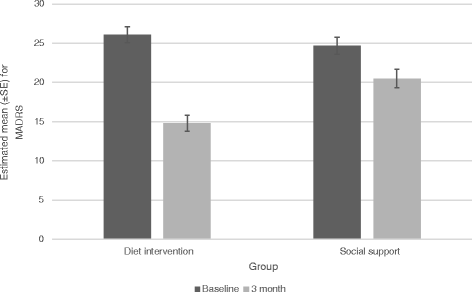
How could this be? It’s no great mystery. Biological mechanisms account for dietary effects on mental health. Cofactors for hundreds of enzymes, nutrients are essential for healthy brain structure and function. They support metabolic pathways, neurotransmitter synthesis, mitochondrial function, and more. Causes of poor physical health, like inflammation, oxidation and impaired blood flow also impact the brain—and are related to unwholesome diets.
The primary cause of disability worldwide, depression is debilitating for sufferers. Maybe it’s time to prescribe good food.
Originally published in Science Nutshell.

